Fascia, revisited
What we actually know, and what yoga teachers can stop worrying about.
For years, fascia has been described as sticky, glued down, dehydrated, or full of adhesions. You have probably heard that we need to release it, break it up, or squeeze toxins out of it.
The problem is that much of that language does not reflect current evidence.
Our understanding of fascia has evolved significantly over the past two decades, particularly through the work of researchers such as Schleip, Stecco, Findley, and others involved in the Fascia Research Congress (Schleip et al., 2012; Findley and Schleip, 2007).
If you teach yoga, this matters. Because the way we talk about tissue shapes the way our students interpret sensation, pain, and their own bodies.
Let’s update the story.
[Premium members - click the play button above the introduction to listen to the audio version of the newsletter and make sure you scroll all the way to the end to download your exclusive printable Quick Reference teaching guide on fascia.]
Three ways to train with me, when you’re ready…
Study live online:
My new Anatomy Applied to Yoga 6-Week Course starts April 21st. Evidence-based training to deepen your understanding of how yoga affects the body. Reserve your spot today.
Train in person:
UK (Mar/Apr), US East Coast (May), UK & Europe (June). Interactive, evidence-based workshops designed to help you teach with clarity and confidence. Book your place (spots limited).
Join the Enlightened Yoga Collective:
Free 1-week trial. On-demand, teacher-focused lessons and a supportive community to help you plan and teach with confidence. Start your free trial.
👉Fascia is not just wrapping
Fascia is a continuous connective tissue network that surrounds, connects, and blends with muscles, tendons, ligaments, joint capsules, and even organs.
It is not separate from muscle. It integrates with it.
Force is transmitted not only through tendons, but also through fascial connections between muscles, a concept known as myofascial force transmission (Huijing, 2009).
In practice, that means the body does not work in isolated pieces.
When you cue a student to press into the floor in Downward Dog, force travels through multiple connected tissues, not just a single muscle.
Fascia is part of that integrated system.
👉Fascia feels
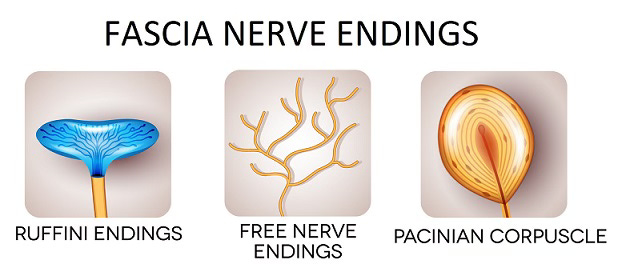
Fascial tissues are richly innervated. They contain sensory receptors that respond to pressure, stretch, and load, as well as nociceptors involved in pain signalling (Schleip et al., 2012).
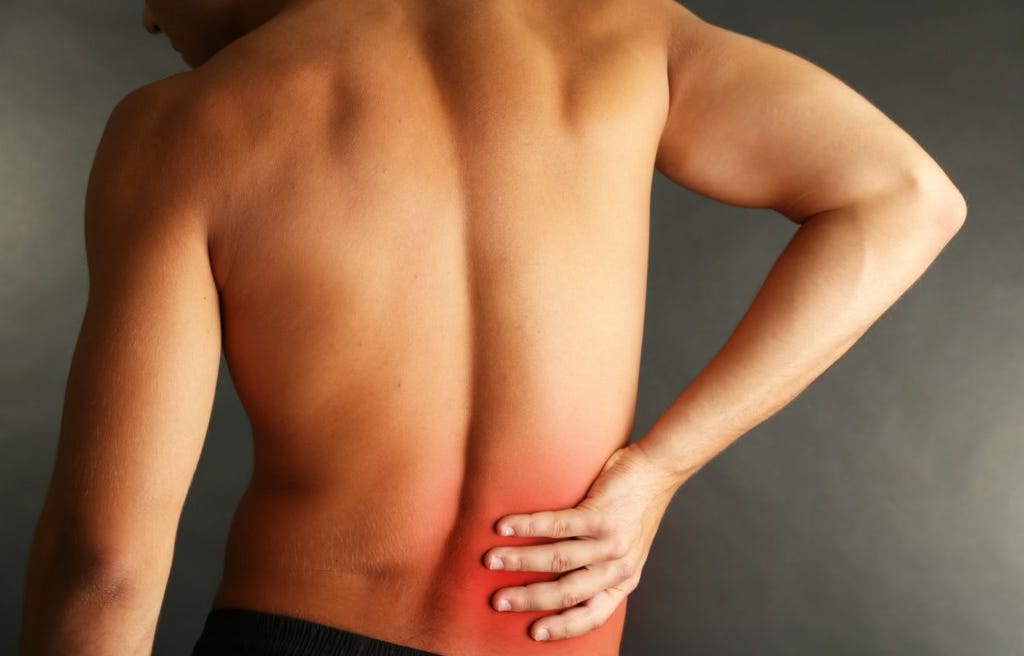
Some layers of fascia, such as the thoracolumbar fascia, have been shown to have high sensory capacity and may play a role in persistent low back pain in some cases (Langevin et al., 2009).
So, when a student says, “I feel this everywhere,” that is not mystical. It is sensory biology.
Slow movement, sustained holds, and novel positions change sensory input. Often the short-term effects we attribute to structural change are actually changes in perception.
That is important, and it is powerful. But it is neurological, not magical.
👉What about fascial adhesions?
This is where things get interesting. The word adhesion is often used casually in yoga spaces to describe any feeling of tightness or restriction.
In medicine, however, an adhesion usually refers to fibrous scar tissue that forms after surgery, infection, or significant trauma. These adhesions can bind tissues together in abnormal ways and may require surgical intervention (Diamond and Freeman, 2001).
In healthy, non-injured tissue, there is very little evidence that everyday stiffness is caused by pathological fascial adhesions.
What we often call an adhesion in yoga is more likely one of the following:
• altered load tolerance
• protective muscle guarding
• increased tissue sensitivity
• reduced movement variability
• deconditioning
Connective tissue does adapt to load. Collagen responds to mechanical input through a process known as mechanotransduction (Ingber, 2006). With progressive, tolerable loading, connective tissues remodel over time.
But this is adaptation, not breaking up knots.
Manual pressure and stretching are unlikely to mechanically disrupt healthy collagen fibres in any meaningful way, given the forces required to alter connective tissue structure (Chaudhry et al., 2008).
In other words, we are not breaking adhesions apart in a yoga class. We are influencing sensation, load tolerance, and movement confidence.
That is still valuable. It is just more honest.
👉Does fascia need “hydrating”?
Fascia contains water-rich ground substance, and movement does influence fluid dynamics.
However, the idea that fascia dries out and must be rehydrated through stretching is an oversimplification.
Movement changes pressure gradients, fluid distribution, and sensory signalling. These changes may alter how movement feels in the short term.
But we are not wringing out toxins or soaking up fluid like a sponge. Again, the effects are largely neurological and mechanical.
👉Fascia and pain
Yes, fascia can be involved in pain. It contains sensory receptors, including nociceptors, specialised nerve endings that detect potential threat such as high pressure, stretch, or inflammation, and send signals to the brain.
But pain is not a simple reflection of tissue tightness.
Pain is an output of the nervous system, shaped by sensory input, context, belief, stress, sleep, and previous experience.
When we say, “Your fascia is tight and causing your pain,” we risk reinforcing a fragile body narrative.
When we say, “This area may be sensitive right now. Let’s explore it gradually,” we reinforce adaptability.
As teachers, we do not just guide movement. We guide meaning.
👉So how should we talk about fascia?
We can move away from dramatic metaphors.
Instead of saying:
“We are breaking up adhesions.”
We might say:
“We are gradually increasing load tolerance.”
“We are exploring range with control.”
“We are helping your system become more comfortable with this position.”
Instead of:
“Your fascia is tight.”
We might say:
“This range feels unfamiliar right now.”
“Let’s see if it feels different with breath and time.”
That shift in language reduces threat. And reducing perceived threat can change pain and performance outcomes in meaningful ways.
👉Why this matters for teachers
Your words shape your students’ beliefs.
If you frame their body as glued together and dysfunctional, they may move cautiously and fearfully.
If you frame their body as adaptable, responsive, and capable of change, they are more likely to move with curiosity and confidence.
Fascia is living tissue. It responds to load. It participates in sensation. It adapts over time. It does not need rescuing. It needs intelligent, progressive input. And thoughtful language.